Tonsillectomy: What Patients Should Know Before the Procedure
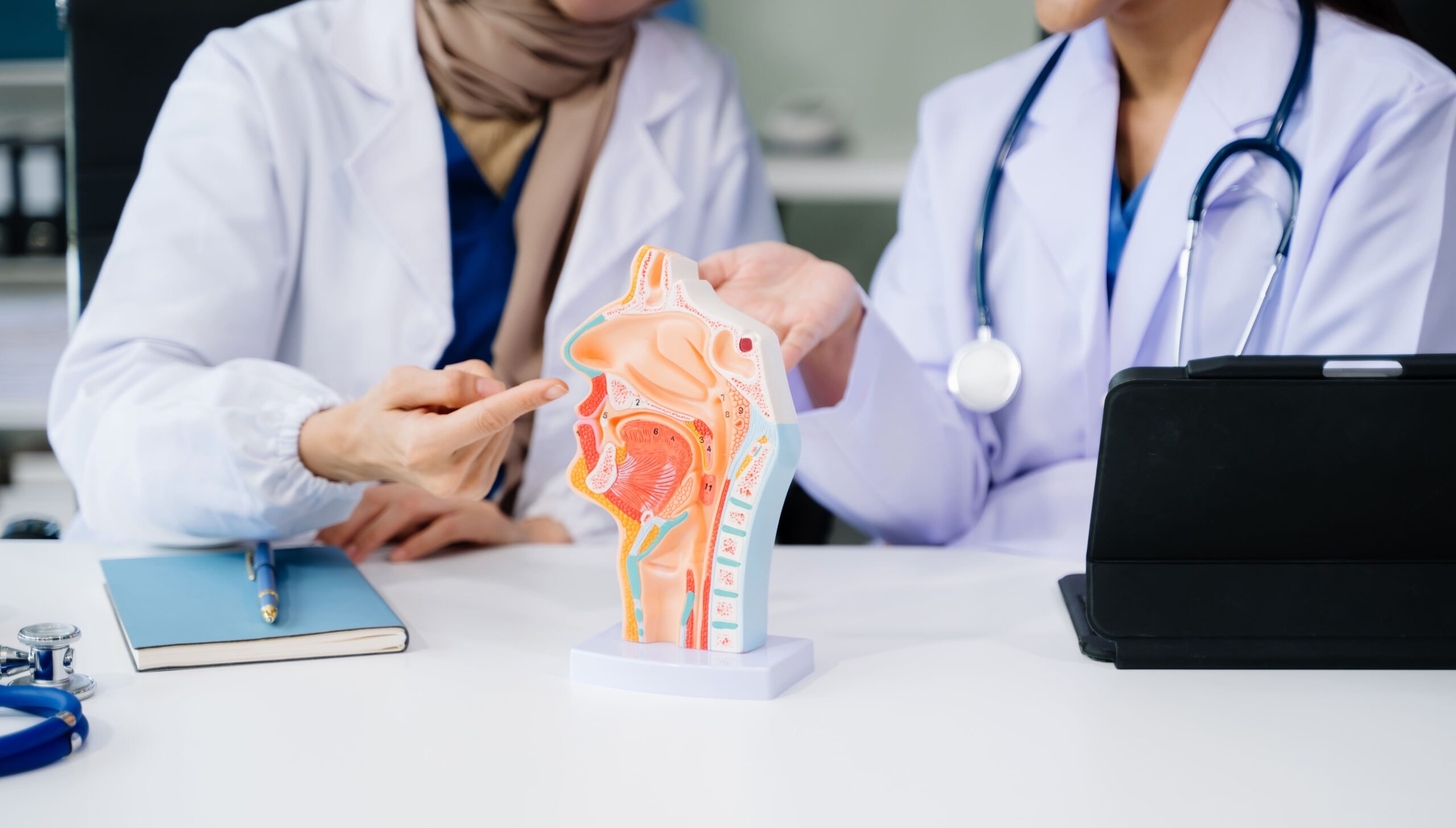
Tonsillectomy surgically removes the palatine tonsils—two tissue masses at the back of your throat that help fight infections. Although tonsils play a role in childhood immunity, removing them in older children and adults doesn’t weaken your immune system, as other tissues take over this function. The procedure is recommended when chronic tonsillar problems—such as recurrent infections or breathing difficulties—significantly affect your quality of life.
Medical Reasons for Tonsillectomy
Recurrent Tonsillitis
Repeated bacterial or viral infections of the tonsils cause significant disruption to daily life, school attendance, and work productivity. Surgeons may recommend tonsillectomy when infections occur with sufficient frequency and severity to justify the risks of surgery and the recovery period. Each infection episode involves:
- Throat pain
- Fever
- Difficulty swallowing
- Often requires antibiotic treatment, which carries its own considerations regarding antibiotic resistance and side effects
The decision involves weighing the ongoing infection burden against the risks of surgical intervention. Your healthcare provider can offer personalised advice based on your individual factors. These include the frequency of documented infections annually, your response to medical treatment, and the degree of functional impairment you experience.
Obstructive Sleep Symptoms
Enlarged tonsils can block the upper airway during sleep, causing breathing disruptions that affect both sleep quality and daytime function.
Common symptoms include:
- Snoring and breathing pauses during sleep (apnea episodes)
- In children: Behavioural issues, attention difficulties, and growth concerns
- In adults: Daytime fatigue, morning headaches, and reduced cognitive performance
- Sleep studies help measure the severity of obstruction and guide treatment decisions. Tonsillectomy may be recommended when enlarged tonsils significantly narrow the airway and contribute to these symptoms.
Other Indications
Tonsillectomy may also be recommended for several other conditions:
Additional reasons for surgery:
- Peritonsillar abscess (pus collection near the tonsil): May require tonsillectomy during the acute episode or as preventive surgery to avoid recurrence
- Asymmetric tonsil enlargement: Requires evaluation to rule out underlying disease; tissue examination after removal provides diagnostic information
- Chronic tonsil stones (tonsilloliths): Small calcified deposits causing persistent bad breath and throat discomfort; surgery is considered when conservative treatments fail
Surgical Techniques
Cold Steel Dissection
Traditional surgical removal uses metal instruments. The surgeon separates the tonsil from the surrounding tissue along natural tissue planes. This technique minimises thermal injury to adjacent structures. The surgeon carefully identifies and controls bleeding from blood vessels during the procedure.
Electrocautery Methods
Electrical current simultaneously cuts tissue and seals blood vessels. This reduces bleeding during the operation. Monopolar and bipolar cautery devices (different types of electrical surgical tools) exhibit distinct characteristics in terms of tissue effect and precision. The thermal energy required for cutting creates a zone of tissue injury. This may influence healing and post-operative discomfort.
Coblation Technology
Radiofrequency energy, when combined with saline solution, creates a plasma field. This dissolves tissue at relatively low temperatures. This approach aims to minimise collateral thermal damage while maintaining tissue removal and haemostasis (the process of stopping bleeding). Recovery characteristics may differ from those of higher-temperature techniques, although individual variation exists.
Intracapsular Tonsillectomy
The surgeon removes part of the tonsil while preserving the tonsillar capsule (the outer layer of tissue surrounding the tonsil). This reduces exposure of the pharyngeal muscles and may decrease postoperative pain and the risk of bleeding. This technique is suitable for selected cases, particularly those performed primarily for obstructive symptoms rather than recurrent infection. Some tonsillar tissue remains. There is a little possibility of regrowth requiring further intervention.
Pre-Operative Preparation
Medical Evaluation
Pre-operative assessment includes review of:
- Medical history
- Current medications
- Allergies
- Previous anaesthetic experiences
Evaluation of blood clotting function identifies patients who require additional precautions. Conditions affecting airway management, cardiovascular function, or wound healing require specific attention. These may influence the anaesthetic approach.
Medications that affect blood clotting must be discontinued before surgery. These include aspirin, nonsteroidal anti-inflammatory drugs (e.g., ibuprofen), and certain supplements. Specific timing depends on the medication’s duration of action and individual patient factors. Herbal supplements, including ginkgo, garlic, and fish oil, may also affect bleeding. You should discuss these with the surgical team.
Fasting Requirements
An empty stomach reduces the risk of aspiration (stomach contents entering the lungs) during general anaesthesia. Standard fasting protocols specify minimum intervals for solid food, clear liquids, and breast milk (for infants). You will receive specific instructions regarding timing based on your scheduled surgery time. Chewing gum and sweets should also be avoided during the fasting period.
Day-of-Surgery Logistics
Arrive at the surgical facility at the designated time. This allows for registration, nursing assessment, and anaesthetic preparation. Wear comfortable, loose-fitting clothing. Remove jewellery, contact lenses, and nail polish (which interferes with oxygen monitoring). Arrange transportation home. Driving after general anaesthesia is unsafe.
The Surgical Experience
Anaesthesia
The procedure is performed under general anaesthesia, which makes you completely unconscious and pain-free while the anaesthetist monitors your heart rhythm, blood pressure, oxygen levels, and breathing throughout surgery. You will remember nothing from the surgical period and will wake up in a monitored recovery area where staff assess your breathing, consciousness, pain levels, and any bleeding before discharge or transfer to the ward.
Procedure Duration
The actual tonsil removal typically takes between 20 and 45 minutes. Duration depends on the technique used, the size of the tonsils, and anatomical factors. The total operating theatre time is longer. This accounts for anaesthetic induction, positioning, and emergence. Some patients require overnight observation. Others meeting discharge criteria return home the same day.
Immediate Post-Operative Period
Throat pain, difficulty swallowing, and sometimes ear pain (referred via shared nerve pathways) begin as anaesthesia wears off. Nausea from anaesthetic medications or swallowed blood may occur. Staff administer pain medication and anti-nausea drugs as needed. Some blood-tinged saliva is normal. Active bleeding requires assessment.
Recovery Timeline and Expectations
First Week
What to expect during early recovery:
- Pain typically peaks mid-week as the surgical site heals and the protective white membrane (eschar) covering the tonsil beds changes
- Regular pain medication is essential to maintain comfort and support adequate fluid intake
- Throat pain may radiate to the ears due to shared nerve pathways (this doesn’t indicate an ear infection)
- Voice changes, mild fever, and bad breath are common and resolve as healing progresses
- Inadequate hydration is a common reason for hospital readmission during this period
Second Week
As healing advances:
- Pain gradually decreases, though the timeline varies between individuals
- Many patients return to a normal diet, though some foods may still cause discomfort
- The white membrane separates from the tonsil beds, which may cause minor bleeding episodes
- Avoid gargling or vigorous throat clearing, as these can disrupt healing tissue
- Your doctor will advise when you can return to work or school based on your recovery progress
Complete Healing
Full tissue healing takes approximately three to four weeks. The area may remain sensitive longer. Scarring occurs at the site of tonsillar removal. The appearance of the throat changes permanently. Dietary restrictions are lifted completely once healing is complete.
Post-Operative Care Essentials
Pain Management
Scheduled pain medication works more effectively than waiting until pain becomes severe. The appropriate medication and dosage should be determined by a healthcare professional based on individual needs and surgical factors. Avoiding aspirin and ibuprofen reduces the risk of bleeding. Some surgeons permit specific non-steroidal medications after the immediate post-operative period.
You may apply ice packs to the neck externally for additional comfort. Sucking on ice chips soothes the throat and helps hydrate. Pain typically increases with swallowing. This creates reluctance to drink that you must overcome to prevent dehydration.
Hydration and Nutrition
Fluid intake takes priority over solid food during early recovery. Cold or room-temperature liquids feel more comfortable than hot drinks. Water, diluted fruit juice, electrolyte solutions (drinks that replace minerals lost through bodily fluids), and non-acidic beverages maintain hydration. Milk-based drinks are acceptable despite traditional concerns about mucus production.
Soft, cool foods provide calories and protein for healing. These include:
- Yoghurt
- Ice cream
- Smooth soups
- Mashed potato
- Soft pasta
Avoid crunchy, sharp, or heavily spiced foods that irritate healing tissue. Acidic foods and drinks may cause a stinging sensation.
Activity Restrictions
Rest significantly during the first week. Gradually increase activity as comfort permits. Avoid strenuous exercise, heavy lifting, and activities that increase the risk of falls or contact for at least two weeks. Elevated blood pressure and trauma increase bleeding risk. Swimming is restricted until healing is complete to avoid infection.
Coughing, sneezing, and nose-blowing generate pressure. This may disrupt healing tissue. Throat clearing should be gentle. Speaking is acceptable, but prolonged vocal use may cause discomfort during early recovery.
What Our ENT Surgeon Says
The recovery period following tonsillectomy requires patience and adherence to post-operative instructions. Pain during the first week is expected and manageable with appropriate medication. The discomfort is temporary whilst the benefits of surgery persist long-term.
Patients who maintain adequate hydration and consistently adhere to activity restrictions experience smoother recoveries with fewer complications. Everyone’s healing trajectory differs slightly. Age, surgical technique, and individual factors influence recovery.
Putting This Into Practice
- Prepare your recovery space before surgery with easy access to medications, drinks, soft foods, and entertainment. Having supplies ready eliminates the need for shopping trips during the most uncomfortable days.
- Track fluid intake using a log or measured container to ensure adequate hydration. Aim for small, frequent sips rather than large amounts at once. Swallowing becomes easier with practice despite initial discomfort.
- Sleep with your head elevated using extra pillows to reduce throat swelling and discomfort. This position also helps manage mild bleeding by preventing blood from accumulating in the throat.
- Use a humidifier in the bedroom to maintain a moist air environment. This helps reduce throat dryness that exacerbates pain. Dry air from air conditioning can be particularly irritating during recovery.
- Schedule follow-up appointments before surgery so they’re already in the calendar. Post-operative review allows assessment of healing and management of any concerns.
When to Seek Professional Help
- Active bleeding from the mouth or nose—more than minor streaking in saliva
- Inability to swallow liquids or medications due to severe pain
- Signs of dehydration: dark urine, dizziness, reduced urination, dry mouth
- Fever persists despite paracetamol
- Difficulty breathing or noisy breathing when awake
- Neck stiffness combined with high fever
- Persistent vomiting prevents fluid intake
- Worsening pain after initial improvement
- Bleeding that stops then recurs
Cost Considerations
Tonsillectomy costs vary depending on:
- Surgical facility (public vs private hospital)
- Anaesthesia and operating theatre fees
- Surgeon’s fees
- Overnight stay requirements
- Post-operative medications
Insurance coverage:
Check with your insurance provider before proceeding, as coverage depends on:
- Whether the surgery is considered medically necessary (usually covered)
- Your specific policy terms and exclusions
- Pre-authorisation requirements
For subsidised options, Singapore citizens may be eligible for surgery at public hospitals with Medisave and government subsidies. Your surgeon’s office can provide detailed cost estimates during consultation.
Commonly Asked Questions
How long does a tonsillectomy take?
The surgical removal typically takes 20-45 minutes, though total time under anaesthesia is longer (usually 1-2 hours) to account for induction, positioning, and emergence. Same-day discharge is common for many patients, whereas others stay overnight based on factors such as age, distance from medical care, and individual recovery responses.
Will I lose my voice permanently?
No. Temporary voice changes result from throat swelling and altered resonance, but the voice typically returns to normal within 2-3 weeks as healing progresses. The tonsils don’t control voice production, so permanent voice changes are not expected from this procedure.
Can tonsils grow back after removal?
Complete tonsillectomy removes all tonsillar tissue, preventing regrowth. Partial tonsillectomy (intracapsular technique) leaves some tissue that can occasionally enlarge. This potentially requires further treatment. Regrowth requiring repeat surgery is uncommon with standard complete removal.
What’s the worst day of recovery?
Pain typically peaks between days 3 and 7. Many patients report days 4 to 6 as the most uncomfortable. This coincides with the separation of the protective membrane covering the surgical site. Pain then gradually decreases over the following week.
Can adults have a tonsillectomy?
Adults undergo tonsillectomy for appropriate indications. Recovery tends to be more prolonged and more uncomfortable than in children. Adult tonsillectomy requires careful consideration of time off work and adequate support during recovery. The procedure itself is technically similar across age groups.
Next Steps
Adequate hydration and adherence to activity restrictions significantly influence recovery outcomes. Prepare your home environment before surgery and understand when complications require medical attention.
If you’re experiencing recurrent throat infections, breathing difficulties during sleep, or chronic tonsil problems, consult an ENT surgeon to determine whether tonsillectomy is appropriate for your condition.