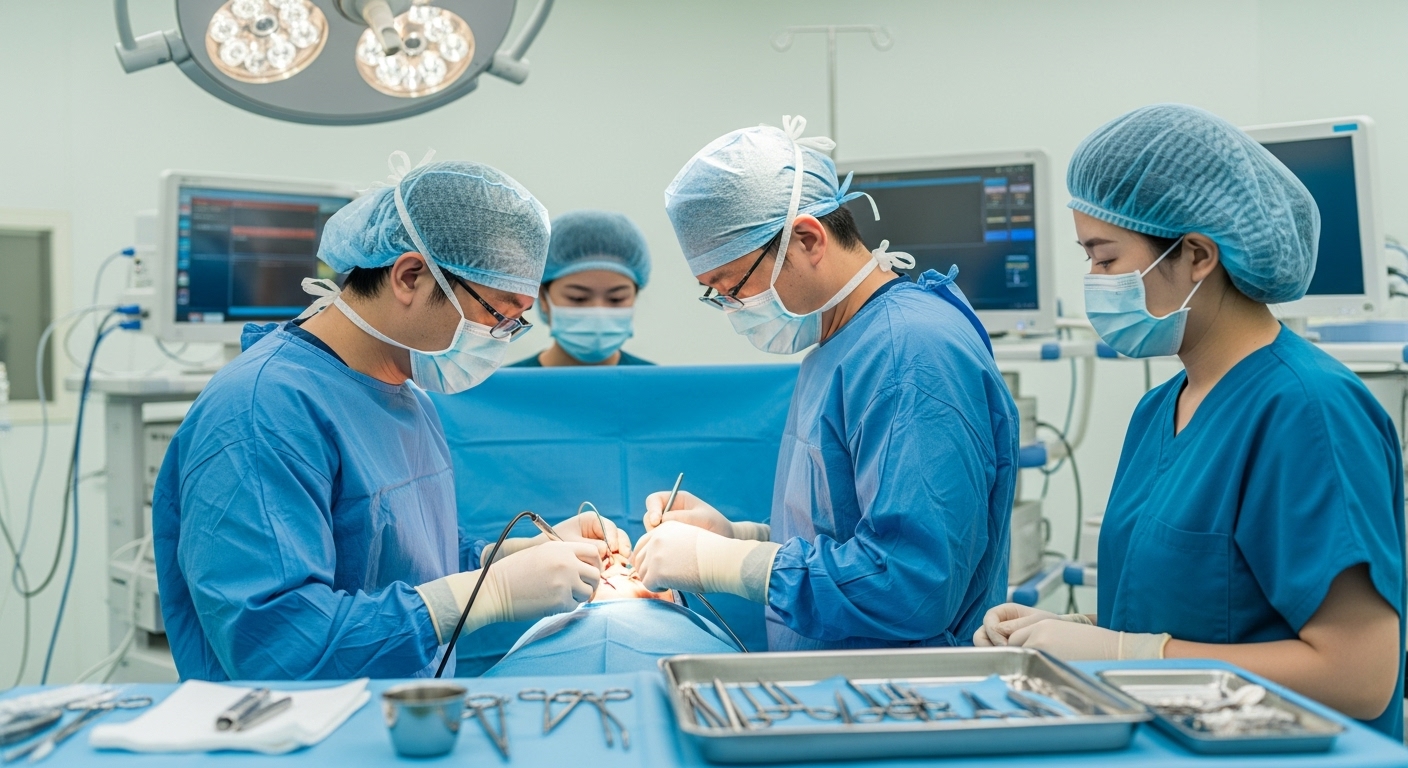
Recovery Guide After Sinus Surgery

Modern endoscopic sinus surgery aims to preserve normal sinus anatomy while removing diseased tissue, unlike older techniques that removed entire sinus walls. These minimally invasive approaches generally cause less tissue trauma, with recovery that typically spans weeks rather than months for many patients.
Recovery experiences vary with the extent of surgery. Individuals undergoing limited procedures may return to desk work within approximately a week, whereas those with more extensive surgery may require up to two weeks to resume normal activities. Post-operative care plays a vital role in supporting healing and may influence outcomes.
First 48 Hours Post-Surgery
In the first two days after surgery, it is normal to experience nasal congestion, light bleeding, and facial pressure. Blood-tinged mucus may drain intermittently — you may gently replace the nasal gauze when it becomes saturated. Sleeping with your head elevated may help reduce swelling and pressure.
Pain usually peaks within the first 12 hours as anaesthesia wears off. Take prescribed pain medication as directed by your healthcare professional before the pain worsens.
If nasal packing or splints were placed during surgery, these may cause a sensation of fullness or congestion until removal, usually within 24–72 hours.
If your sinus clearance was performed alongside Deviated Septum Surgery in Singapore, you may have internal splints to support the straightened midline. These are typically removed during your first post-operative visit to significantly improve nasal airflow.
Applying cold compresses to the cheeks or forehead for short intervals may help reduce swelling, provided your doctor has approved it. Avoid blowing your nose or forceful sneezing to help protect healing tissues.
Week 1: Initial Healing Phase
Days 3-7 mark the transition from acute to early healing phases. Congestion often worsens before improving as blood clots and mucus accumulate in the nasal passages. Because Functional Endoscopic Sinus Surgery Singapore focuses on restoring natural ventilation, you may experience temporary congestion as the internal tissues heal. Following your. Saline rinses begin after packing removal, typically starting on day 3.
Nasal Irrigation Technique
Mix distilled or boiled, cooled water with the provided saline packets; do not use tap water directly. Lean over the sink at a 45-degree angle, insert the irrigation bottle tip into one nostril, and squeeze gently. Solution flows through the nasal passages and exits the opposite nostril.
Your healthcare professional should determine the frequency and technique for rinses.
Initial rinses may produce blood clots, thick mucus, and debris; this typically indicates effective cleaning rather than complications. Rinse volume increases gradually as swelling decreases. Some patients experience ear popping during irrigation; pause and swallow to equalise pressure.
Activity Restrictions
Avoid bending below waist level, lifting objects over 10 pounds, or straining during bowel movements. These activities increase blood pressure in head vessels, potentially triggering bleeding. Consult your healthcare professional regarding stool softeners if constipation develops from pain medications.
Light walking promotes circulation and reduces the risk of blood clots. Start with 5-minute sessions and increase gradually. Avoid strenuous exercise, swimming, or other activities that cause heavy breathing for the duration recommended by your healthcare professional.
Return to work depends on job requirements: desk work often resumes at 7 days, whereas physical labour requires a more prolonged recovery. Driving resumes once pain medication is discontinued and head movement is comfortable, typically on days 3-5. Consult your healthcare professional for specific guidance on activity resumption.
Weeks 2-4: Active Recovery
Crusting peaks during weeks 2-3 as healing tissues shed debris. Hard crusts form along incision sites and feel obstructive despite improved airflow. Avoid picking or forceful blowing; crusts naturally soften and dislodge with consistent saline rinses.
Debridement Appointments
The success of your recovery depends heavily on clinical monitoring. Regular reviews with a Nose & Sinus ENT Specialist in Singapore allow for the gentle removal of surgical crusting and ensure that the sinus passages are healing without scarring or adhesions.”
ENT follow-ups at weeks 1, 3, and 6 include endoscopic cleaning. The surgeon removes crusts, blood clots, and scar tissue using specialised instruments. Debridement is uncomfortable but rarely painful; topical anaesthesia numbs the tissues before cleaning.
Post-debridement breathing improves. Some bleeding occurs for 24 hours after cleaning. Continue regular saline rinses between appointments to minimise crust formation.
Medication Management
Antibiotics are administered for 7-14 days, depending on the extent of the surgery and the risk of infection. Complete the full course even if symptoms improve. Oral steroids reduce inflammation for 5-7 days post-surgery and are tapered in accordance with the prescribing physician’s instructions.
Topical steroid sprays are initiated after initial healing, typically at week 2. Aim sprays away from the septum toward the outer nasal walls. Steroid rinses may replace sprays for patients with extensive polyp disease.
Pain transitions from constant to intermittent by week 2. Facial pressure sensations persist longer than sharp pain. Over-the-counter pain relievers usually suffice after day 7.
Managing Common Symptoms
Nasal Congestion
Congestion fluctuates throughout recovery, often worse in the mornings due to overnight mucus accumulation. Humidified air may help prevent excessive drying; run a cool-mist humidifier continuously in your bedroom. Avoid decongestant sprays unless prescribed by a healthcare professional, as rebound congestion complicates healing.
Patients who underwent Inferior Turbinate Hypertrophy Treatment in Singapore as part of their sinus surgery will notice a gradual reduction in nasal swelling over 4 to 6 weeks. Proper allergy management during this time helps prevent the turbinates from re-enlarging.
Steam inhalation may provide temporary relief. Inhale steam from a shower or lean over a hot bath with a towel tent for 5-10 minutes. Add prescribed medications to steam if directed by your healthcare provider.
Fatigue and Sleep Disruption
Surgical healing demands significant energy. Fatigue persists for several weeks despite adequate rest. Schedule afternoon naps and avoid overcommitting to activities. Sleep quality is affected by mouth breathing and positional requirements.
Use saline gel or spray before bed to help minimise overnight drying. A mouth spray may help prevent dry mouth from constant mouth breathing. Multiple pillows or a wedge may help maintain head elevation while reducing neck strain.
Smell and Taste Changes
Olfactory function decreases temporarily due to swelling and crusting. Patients typically notice gradual improvement, with full recovery taking several weeks. Taste relies heavily on smell, so food may seem bland during early recovery.
Zinc supplements may support olfactory recovery; discuss with your healthcare provider before starting. Strong odours like perfumes or cleaning products may trigger discomfort during healing.
Complications Requiring Medical Attention
Contact your ENT specialist immediately for:
- Bleeding soaking more than one gauze pad per hour
- Vision changes or eye swelling
- Headache unresponsive to pain medication
- Fever above 38.5°C persisting over 24 hours
- Clear fluid draining from the nose (possible CSF leak)
- Increasing pain after initial improvement
- Purulent discharge with foul odour
Long-Term Recovery Expectations
Healing continues gradually over several months as tissues remodel and inflammation subsides. Many patients notice a gradual improvement in breathing and sense of smell.
Continue maintenance care such as saline rinses and prescribed nasal sprays to support long-term sinus health. Avoid swimming in chlorinated or natural water sources until cleared by your surgeon.
Follow-up endoscopic examinations at regular intervals help with proper healing and early detection of scar tissue.
Did You Know?
Endoscopic sinus surgery preserves normal sinus anatomy while removing diseased tissue, unlike older techniques that removed entire sinus walls. This preservation allows sinuses to resume normal function after healing.
Putting This Into Practice
- Develop a medication schedule with phone alarms for antibiotics, analgesics, and rinses.
- Prepare your recovery space with extra pillows, a humidifier, tissues, and gauze before surgery.
- Stock up on soft foods and prepare meals in advance for the first week.
- Arrange transportation for the first few days while taking pain medication.
- Set up a rinse station in your bathroom with distilled water, saline packets, and clean towels.
When to Seek Professional Help
- Sudden vision loss or double vision
- Neck stiffness with headache
- Clear watery discharge that increases when bending forward
- Bleeding requiring constant gauze changes for over 2 hours
- Facial swelling extending to the eyes
- High fever with confusion or fatigue
- Persistent vomiting is preventing medication intake
Commonly Asked Questions
When can I resume normal nasal blowing after surgery?
Gentle nose-blowing resumes after 2 weeks in most patients. Start with light pressure and block one nostril at a time. Full-force blowing is done in weeks 4-6, when tissues are fully strengthened. Your surgeon provides specific timing based on your healing progress.
Why does my sense of smell seem worse after surgery?
Swelling and crusting temporarily block odour molecules from reaching smell receptors. Additionally, surgical trauma causes temporary nerve stunning. Smell typically returns gradually over 4-8 weeks as swelling resolves and nerves recover.
Can I fly after sinus surgery?
Air travel requires surgeon clearance, typically after 2-3 weeks. Pressure changes during flight may cause discomfort or bleeding in early recovery. Use a saline spray before and during flights. Avoid flying with active sinus infections.
Will I need to use nasal rinses forever?
Many patients benefit from continued daily rinses, especially those with allergies or chronic sinusitis. Others reduce frequency to several times weekly or use rinses only during allergy seasons or upper respiratory infections.
How do I know if scar tissue is forming?
Progressive congestion returning after initial improvement suggests the formation of scar tissue. Difficulty with nasal rinses flowing through previously open passages indicates obstruction. Regular follow-up endoscopies detect and address scar tissue before symptoms develop.
Next Steps
Consistent postoperative care and follow-up appointments may facilitate smoother healing and reduce the risk of complications. If you experience persistent sinus symptoms or concerns about recovery, consult a qualified ENT specialist for assessment and advice.